Indications
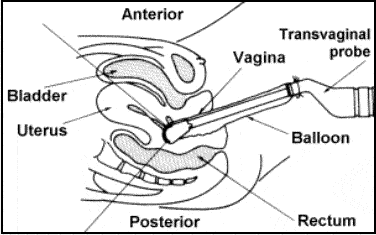
A saline sonography (SSH) is routinely done to make sure that the endometrial cavity (inside of the uterus) appears normal. Benign growths such as endometrial polyps or uterine fibroids may develop in the cavity and create an environment that is hostile for implantation. These conditions can usually be diagnosed by SSH. Scar tissue may also be identified. SSH may be done as part of an evaluation for recurrent pregnancy loss or done prior to an IVF cycle. It may also be done to evaluate causes of irregular or very heavy menstrual cycles and some types of chronic pelvic pain.
Scheduling
Our physicians perform this procedure in the office. We will schedule this procedure for you with one of our physicians. SSH is usually done early in the cycle, just after the period stops but before ovulation. It is important to remember that you should not be bleeding at the time of the procedure so be careful to avoid scheduling during your menses. You will be able to drive yourself home so you do not have to have someone else with you.
Preparing for a Saline Sonohysterogram
- We may advise you to take antibiotics on the day before, the day of, and the day after this procedure. We will give you a prescription.
- The procedure may occasionally cause mild cramping so it is a good idea to take 400 to 800 mg of ibuprofen (Motrin) or 2 Aleve tablets with a light snack approximately 60 minutes prior to your procedure. This is not essential if these types of medications bother your stomach.
The Procedure
The procedure is simple and usually takes less than 5 to 10 minutes. The following steps are representative of a typical procedure:
- A speculum is inserted into the vagina and the cervix is cleansed with an antiseptic swab.
- The catheter – which is about the 1mm (the diameter of a single spaghetti strand) is inserted and slides through your cervical canal. A small balloon is then inflated in the canal with up to 1 teaspoon of water to hold it in place.
- The ultrasound probe is placed in the vagina.
- Sterile salt water solution (saline) flows through the cannula and into the uterine cavity. This distends the endometrial cavity and allows the physician to see the entire cavity on the ultrasound monitor. (Normally the two sides of the endometrium touch and there is very little volume – analogous to a collapsed balloon, making it much more difficult to see any abnormalities of the cavity). This may cause mild cramping.
- Several images will be taken of your uterus during the procedure. Your physician may also take ultrasound images of your ovaries.
- Any abnormalities will also be noted. If any abnormalities are found, it may be necessary to schedule another procedure, known as a hysteroscopy. (Hysteroscopy consist of a scope, about the size of a ballpoint pen, which is inserted into the uterine cavity. Special instruments designed to work through the hysteroscope are then used to correct the uterine cavity. This is generally done in the hospital because of the anesthesia requirements).
- At the completion of the procedure all the instruments are removed.
What to Expect Afterwards
After the procedure you may continue to have mild cramps for several minutes. You may also have some light spotting or watery discharge and even continued cramping for as long as 24 hours. You should refrain from intercourse for approximately 48 hours. Other than that, you may immediately resume normal activity.

Advanced Reproductive Medicine & Gynecology of Hawaii
Helping to Create New Beginnings